The human body often communicates internal problems through symptoms that seem unrelated to the original source of illness. Many serious diseases begin quietly, producing subtle changes long before clearer signs appear. Because of this, certain physical symptoms may serve as early clues that something deeper is affecting the body.
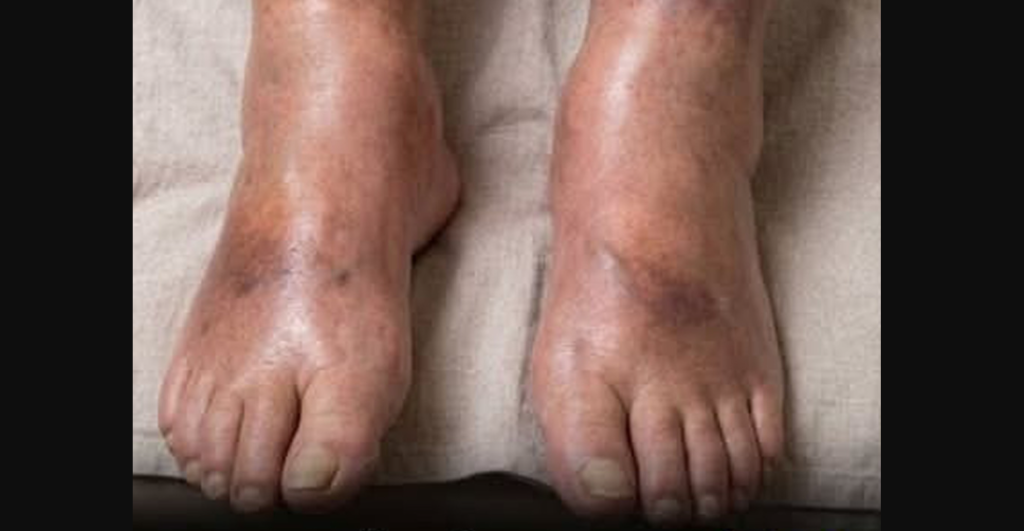
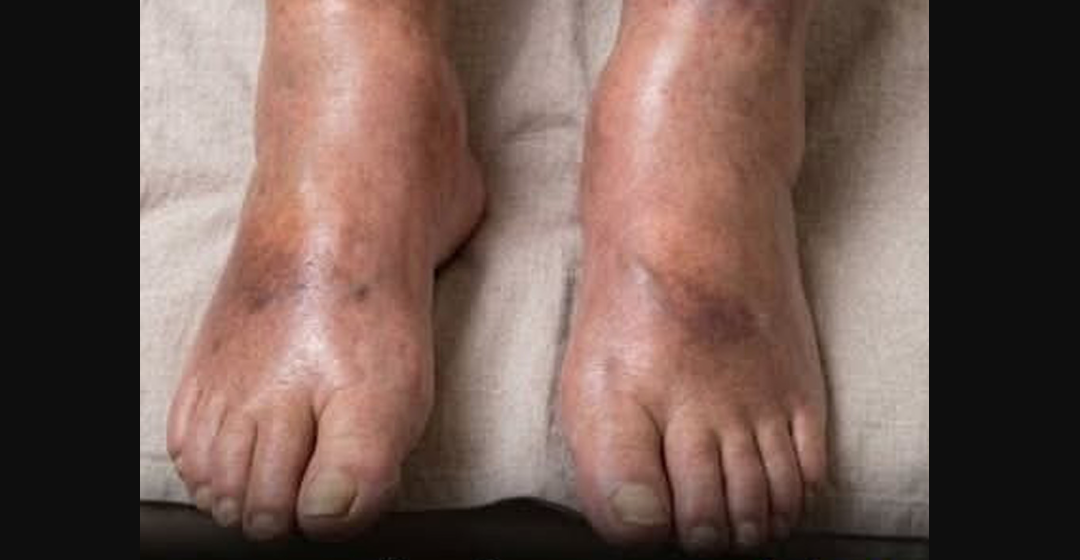
One symptom that sometimes attracts medical attention is swelling in the lower legs. This condition, commonly known as edema, occurs when fluid accumulates in body tissues. Swollen legs are frequently linked to circulation issues, kidney disorders, heart conditions, or prolonged standing. However, in certain situations, physicians investigate additional possibilities when swelling appears suddenly or persists without a clear explanation.
The pancreas plays an important role in digestion and blood sugar regulation. Positioned deep within the abdomen behind the stomach, this organ often develops diseases that remain unnoticed during early stages. Because of its location and the subtle nature of early symptoms, pancreatic conditions can progress quietly before detection occurs.
Researchers continue studying how changes in the body may reveal clues about underlying diseases. One area of interest involves the relationship between leg swelling and blood clot formation, particularly a condition known as deep vein thrombosis.
Understanding Deep Vein Thrombosis
Deep vein thrombosis, often abbreviated as DVT, occurs when a blood clot forms within a deep vein. The condition most commonly develops in the legs, where blood flow moves more slowly compared with other parts of the body. When a clot blocks circulation in these veins, symptoms may appear quickly.
Typical signs of deep vein thrombosis can include swelling in one leg, warmth in the affected area, discomfort, or changes in skin color. In some situations, swelling may be the most noticeable symptom. Medical professionals treat DVT as a serious condition because clots may travel through the bloodstream and affect other organs.
Physicians investigate the cause of such clots carefully, particularly when they occur without an obvious trigger such as surgery, injury, or extended immobility.
The Relationship Between Blood Clots and Cancer
For many years, doctors have recognized that certain cancers may increase the risk of blood clot formation. This relationship was first observed in the nineteenth century by French physician Armand Trousseau, who noticed that some patients developed unexplained clots before their cancers were discovered.
This phenomenon eventually became known as Trousseau syndrome. Modern research has helped clarify the biological processes involved.
Certain tumors release substances into the bloodstream that influence the body’s natural clotting system. These substances can stimulate platelets and other components of blood to activate clot formation more easily than usual. As a result, individuals with some types of cancer may face a higher likelihood of developing blood clots.
Scientific studies continue examining these interactions in order to improve early detection and patient care.
Why the Legs Are Often Affected
Blood flow in the legs travels upward toward the heart, working against gravity. Because of this, circulation through the deep veins of the legs naturally moves more slowly than in many other areas of the body. This slower flow makes the legs particularly vulnerable to clot formation.
When clot-promoting signals circulate through the bloodstream, they often affect these veins first. A developing clot may interrupt normal circulation and cause swelling or inflammation in the surrounding tissue.
Some individuals experience pain, redness, or warmth in addition to swelling. Others notice swelling alone, which may lead them to seek medical evaluation.
Additional Causes of Leg Swelling
Blood clots represent one possible explanation for swelling in the legs, though many other medical conditions can produce similar symptoms. Physicians frequently consider a variety of factors when evaluating this condition.
Heart disease can affect the body’s ability to circulate blood efficiently, leading to fluid buildup in the lower limbs. Kidney disorders may disrupt fluid balance, resulting in swelling. Liver disease can also influence protein levels in the bloodstream, which affects how fluid remains within blood vessels.
In some cases, swelling appears gradually in both legs due to changes in protein levels or circulation. This condition, known as systemic edema, may occur when the body’s fluid balance becomes disrupted.
Because several conditions can cause swelling, medical professionals evaluate the symptom carefully before reaching a diagnosis.
Diagnostic Approaches
When leg swelling appears suddenly or without a clear cause, physicians often begin with diagnostic testing. Blood tests may measure markers that indicate whether the body is forming or dissolving clots.
Imaging studies frequently follow. One commonly used technique is duplex ultrasound, which allows doctors to observe blood flow through the veins. This method can identify clots that block circulation in the legs.
If a clot appears without a known explanation, doctors sometimes recommend additional imaging studies to investigate possible underlying causes. These evaluations help determine whether other medical conditions require attention.
Importance of Early Medical Evaluation
Medical professionals emphasize that leg swelling should never be ignored when it appears unexpectedly or persists for an extended period. Although many causes of swelling are treatable, timely evaluation helps prevent complications and ensures that serious conditions receive appropriate attention.
Healthcare providers assess several factors during evaluation, including medical history, lifestyle habits, and accompanying symptoms. Age, smoking history, unexplained weight loss, and other health changes may guide further investigation.
Treatment and Supportive Care
When deep vein thrombosis is diagnosed, treatment typically involves anticoagulant medications that reduce the blood’s tendency to clot. These medications help prevent existing clots from growing and reduce the likelihood of new clots forming.
Supportive measures may also help relieve swelling and improve circulation. Physicians sometimes recommend compression stockings, elevating the legs during rest, and maintaining gentle physical activity such as walking.
These strategies assist circulation while medical treatment addresses the underlying cause.
Listening to the Body’s Signals
The body often communicates important information through physical symptoms. Changes that seem minor at first can occasionally signal deeper health concerns. Paying attention to these signals allows individuals to seek medical advice when necessary.
Swelling in the legs can arise from many conditions, most of which have clear explanations and effective treatments. At the same time, healthcare professionals encourage individuals to remain attentive to unexplained symptoms.
Early evaluation, open communication with medical providers, and awareness of bodily changes all contribute to maintaining long-term health.
By recognizing the body’s signals and seeking guidance when needed, individuals can take proactive steps toward protecting their well-being and addressing potential concerns in a timely manner.